How are expectations, placebos, and placebo and nocebo effects linked? © kues1/stock.adobe.com
How are expectations, placebos, and placebo and nocebo effects linked? © kues1/stock.adobe.com
Frequently asked questions
Our life is determined by expectations, which fluctuate between hope and fear, but how positive or negative these expectations are largely depends on experiences we have had and remembered. This applies to all areas of life, including medicine, and it is these expectations and previous experiences that patients take with them when they go to a doctor or therapist. Researchers have known for a long time that these expectations can influence physical symptoms, the course of a disease and the efficacy of treatments. Patients experience what are known as placebo effects. In our research, we are working on identifying specific psychological and neurobiological mechanisms so they can be used systematically to benefit patients. The following questions should help to explain how expectations, placebos and placebo effects are linked.
The placebo effect is a positive physical or psychological change that occurs after taking medication without an active ingredient, or after a sham treatment such as simulated surgery or infusion of a simple saline solution. It also plays a role in conventionally prescribed, intrinsically effective (e.g. pharmacologically active) treatments, as positive expectations can influence the outcome of treatment and the pharmacological efficacy of medication. The term "placebo" comes from Latin and means "I shall please".
Expectation effects are no coincidence, but instead based on complex psychoneurobiological processes in the brain. Simply believing that a certain treatment is effective has been shown to activate mechanisms in the body that improve the treatment outcome. This can be described as a kind of "internal pharmacy". Imaging techniques can be used to show that certain areas of the brain, e.g. pain relief systems, are activated during this process. In the field of pain therapy, the placebo effect has been particularly well researched. If a patient expects a remedy or medication to relieve pain, pain-relieving substances, known as endogenous opioids, are released in the brain and can even alter onward transmission of the pain stimulus in the spinal cord. This relieves pain, for example back pain, even though the patient has not taken an opioid analgesic. The specific mechanisms of action underlying such placebo effects on mental illnesses, such as depression, or other physical conditions, e.g. involving the immune system, and how patient expectations can be used systematically to improve medical treatments are the focus of the research undertaken by the interdisciplinary team at our collaborative research centre (CRC) "Treatment Expectation", which is funded by the German Research Foundation.
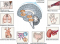
Positive expectations and previous experiences activate complex processes in certain areas of the brain, and these interact with physical processes. The effects can then be detected in various parts of the body, including the immune system, heart, bowel, skin and brain. Expectations have particularly significant effects on pain and depression, and that is why our research focuses on this area. Collaborative Research Centre/Transregio (CRC/TRR) 289 "Treatment Expectation" is investigating which specific mechanisms underlie these effects in the brain and body and how they influence the efficacy of medical treatments.
© Enck P, Bingel U, Schedlowski M, Rief W (2013). The placebo response in medicine: minimize, maximize or personalize? Nature Reviews I Drug Discovery 12: 191-204.
Placebos work, but the effects vary from person to person, symptom to symptom and disease to disease. Genetic factors certainly play a role, but personality traits could also be important. Some people are inherently optimistic, positive and open-minded, whereas others are more anxious, sceptical and critical. Individual expectations and past experience of medication or other treatments are particularly important. In some cases, there is even a placebo effect when patients know they are taking a pill without an active ingredient. This gives us an idea of how powerful these mechanisms can be.
More attention should be paid to the power of expectation in medicine than has previously been the case because it has been shown to help maximise the efficacy of medication and other treatments.
The potent analgesic remifentanil is a very impressive example of this. Positive treatment expectations made it twice as effective at relieving pain, whereas negative expectations, coupled with worry that the pain could get worse, ensured that it lost its effect. Such effects are not limited to pain medication.
These study results seem to explain why some people with chronic diseases do not respond well to pain medication. They are often desperate and anxious, and have lost faith in medicine. This can reduce or even, as in our study, completely reverse the effect of medication that is actually effective. In future, doctors should pay more attention to the previous experiences and expectations of their patients when selecting treatments. The aim must be for patients to start treatment with positive expectations. If necessary, these expectations must be raised with psychological support.
These findings are also of interest to the pharmaceutical industry when developing new approaches to treatment, and this applies to active ingredients, pharmaceutical form, dose and patient information. For example, positive patient expectations could reduce the required dose of a medication and therefore minimise the risk of side effects. The placebo effect can also accelerate healing after surgery, manual therapy and psychological interventions. How exactly it does this and under what conditions is the focus of research.

The bar chart shows the efficacy of potent analgesic remifentanil in patients with different expectations or influenced by different factors. It varies considerably, depending on whether the patient receives the infusion with no expectations, positive expectations or negative expectations of the medication. Positive expectations make it more effective, whereas negative expectations can reverse its effect, as if the patient had not taken any medication at all.
© Bingel U, Wanigasekera V, Wiech K, Mhuircheartaigh R, Lee MC, Ploner M, Tracey I (2011) The effect of treatment expectation on drug efficacy: imaging the analgesic benefit of the opioid remifentanil. Science Transl Med (3)70:70ra14.
Communication and medicine are closely interwoven. Unfortunately, not all doctors make conscious use of opportunities to enhance treatment. How does a doctor, physiotherapist or nurse discuss treatment with the patient? What are their exact words? How crucial are gestures and facial expressions? Communication with patients has been shown to affect whether and how well medication works and how well it is tolerated. Patients who are convinced by a treatment usually benefit more from it. It is therefore important for doctors to take the time to build trust and explain the objectives and benefits of the treatment to patients.
It can only influence processes that the body can trigger itself. Particularly in pain therapy or patients with neurological or psychiatric diseases, such as Parkinson's disease, anxiety or depression, the effects are relatively large. However, placebo effects are not limited to subjective feelings and symptoms such as pain or mood. They can affect many physiological processes from respiration and digestion to the immune system.
This means that they can also support treatment and healing in patients with severe physical illnesses or injuries, but only in combination with established and proven gold-standard treatments.
Treatment can be influenced by negative as well as positive expectations. This is called a nocebo effect (Latin for "I shall harm"). If a patient discovers, for example, that a certain medication has been tolerated poorly by someone they know, the medication is more likely to be less effective or cause side effects in this patient. Studies indicate that the nocebo effect also triggers processes in the central nervous system that can lead to physical changes. In this system, fear of pain can, for example, block opioids and inhibit the messenger dopamine, leading to increased rather than decreased conduction and perception of pain. The nocebo effect probably plays an even greater role in everyday life than the placebo effect but is much less well researched. This is partly for ethical reasons, as deliberately triggering negative patient expectations often pushes the boundaries of medical ethics.
Likewise with the nocebo effect, it is important for medics to realise how communication and positive expectations influence treatment outcome. Just the way a doctor phrases something plays a key role. You can either tell the patient that 10 per cent of people experience side effects or that 90 per cent of people tolerate the medication very well. It is not about withholding or sugar-coating information, but instead sharing it in a way that makes patients less anxious.
Yes, because understanding placebo and nocebo effects has far-reaching implications for the design and interpretation of clinical studies, in which new medications and treatments are often compared with a placebo. One of the fundamental assumptions in these studies is that the placebo and medication have additive effects. However, there is clear evidence that in many cases this fundamental assumption is false. We must therefore have a much better understanding of how to combine the neurobiological effects of positive expectations with the pharmacological effect of medication and how to optimise the interaction of these two factors in order to maximise the efficacy of medication. To achieve this, completely new study designs are necessary because these effects can have a significant impact on study results for a wide variety of pharmaceuticals.

This diagram shows two ways in which the effect of medication could respond to the placebo effect: either the placebo effect (triggered partly by patient expectations) is added to the effect of the medication (left) or the two effects increase multiplicatively (right). The latter would mean that a lower dose of the active substance had the same efficacy as a result of interaction with the placebo effect.
© Enck P, Bingel U, Schedlowski M, Rief W (2013) The placebo response in medicine: minimize, maximize or personalize? Nature Reviews I Drug Discovery 12:191-204
A very clear distinction must be made between the two. Placebos can be effective in the treatment of pain as well as many other symptoms and diseases. That has long been known from relevant experimental and clinical studies. However, there is a dilemma here, in that patients in these situations are left in the dark about the placebo treatment. This is hard to justify from an ethical and legal perspective.
Open-label placebos (OLPs), where the nature of the placebo treatment is explained to patients, offer a way out of this dilemma. Surprisingly, several independent studies of different pain disorders indicate that this kind of OLP treatment can have a positive effect on pain, physical function and quality of life. There are also encouraging results for other indications, such as depression or chronic exhaustion (known as chronic fatigue syndrome).
That is why intensive research into how OLPs work, which patients in particular benefit from them and how they could be used in routine clinical practice is currently being undertaken.
That is a very interesting question for researchers and the reason why such intensive research is being undertaken in this area. Subconscious expectation and learning processes, in particular, are being discussed.
How OLPs have a clinically significant effect, and particularly in whom, is currently being studied both within and beyond the collaborative research centre "Treatment Expectation". From our studies we draw the following conclusion for clinical practice: Despite encouraging early findings for open-label placebos, placebos are first and foremost a tool used in both randomised controlled and experimental studies. How important a role open-label placebos will play in routine treatment is difficult to say at present.
17% of Germans, 12 million people, suffer from long-lasting chronic pain. In her presentation at the DGN (German Society of Neurology) Congress in 2020, Prof. Ulrike Bingel, Director of the Back Pain Centre at Essen University Hospital, explained how precision medication helps and what role psychological and physiotherapeutic factors play. Studies show how open-label placebos can also relieve pain and improve function and mood when used in pain therapy.
© DGN/DGN-Kongress 2020
